Claim Scrubber
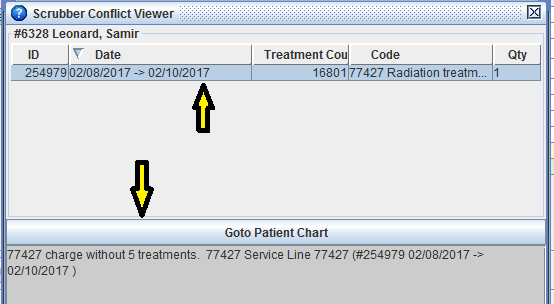
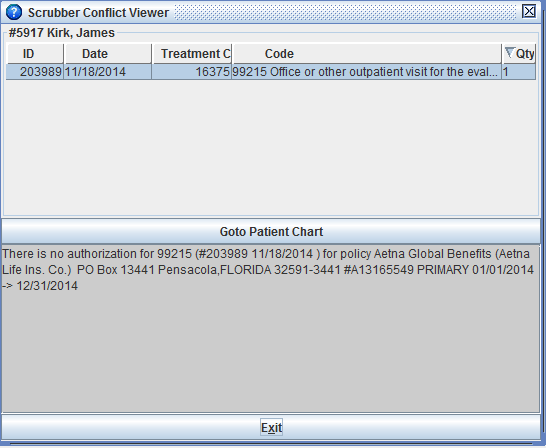
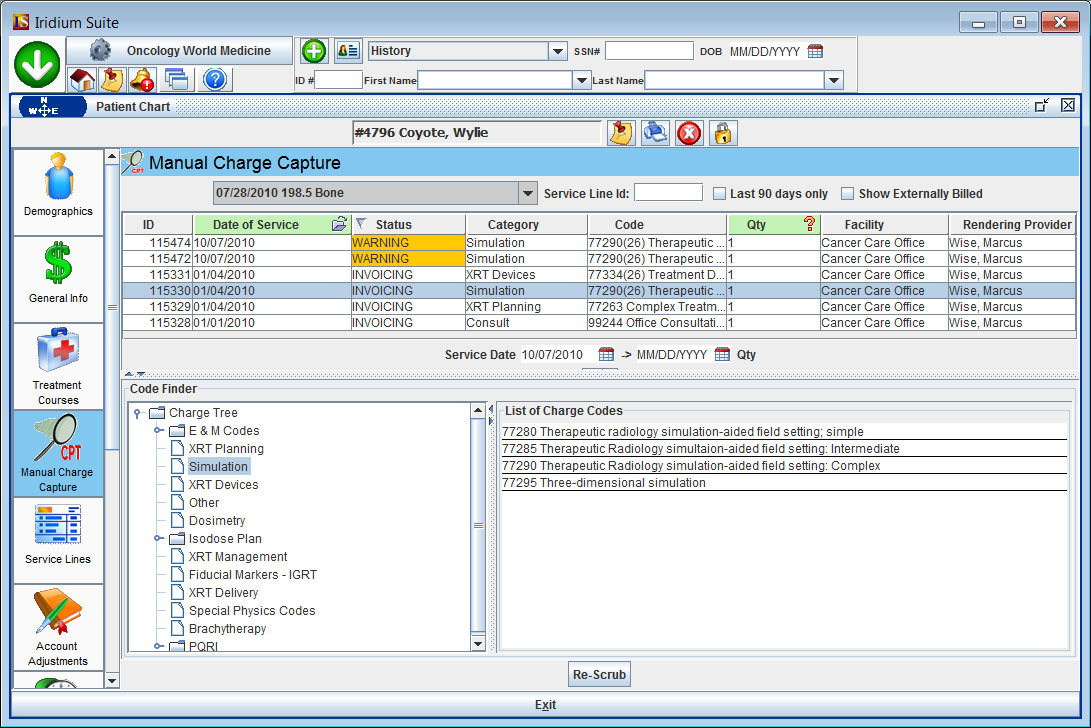
Shavara's claim scrubber, a powerful built-in feature in Iridium Suite, checks codes against billing rules and gives instantaneous feedback, helping coders bill accurately the first time. The system proactively audits charge capture, providing warnings and information about violations of common billing rules before posting charges. Shavara's claim scrubber is customizable, rules can be created sensitized to local, regional payer guidelines and to track unique practice workflows.
Shavara has learned a lot in its 12+ years of dedicated focus in Radiation Oncology. We have listened to our users and incorporated many features and capabilities into Iridium Suite. This foundation of knowledge is our 'experience capital', the know-how we apply to solve gaps and vulnerabilities affecting the revenue cycle process.
In fact, several built-in Iridium Suite capabilities have measureable market potential as standalone bolt-on solutions:
- Shavara claim scrubber
- Shavara Connectivity Clearinghouse
Shavara's customizeable Claim Scrubber is one of several break-out capabilities emerging from our foundation of 'experience capital'.
Ready to learn more...Shavara's Claim Scrubber is your path to Revenue Cycle Management: accomplished.
Iridium Suite Features
Medical billing is complex.
Radiation oncology billing is extremely complex.
Radiation oncologists are some of the highest paid specialists.
It is precisely for this reason the regulators have deliberately made and continue to make changes to the billing workflow to trip up the billers, to slow down the revenue cycle, to penalize the highest earners.
Iridium Suite, a Practice Management software application, is engineered with a keen understanding of the coding and billing process in Radiation Oncology.
Targeting: Free-standing cancer centers, independent physicians tied to Hospital/enterprise settings requiring professional coding and billing capabilities.
Iridium Suite - purpose-built to solve the challenges and complexities of Radiation Oncology coding and billing.
Revenue Cycle Management: Accomplished.